Robotics in Healthcare: Reducing Surgical Errors by 20% by 2026
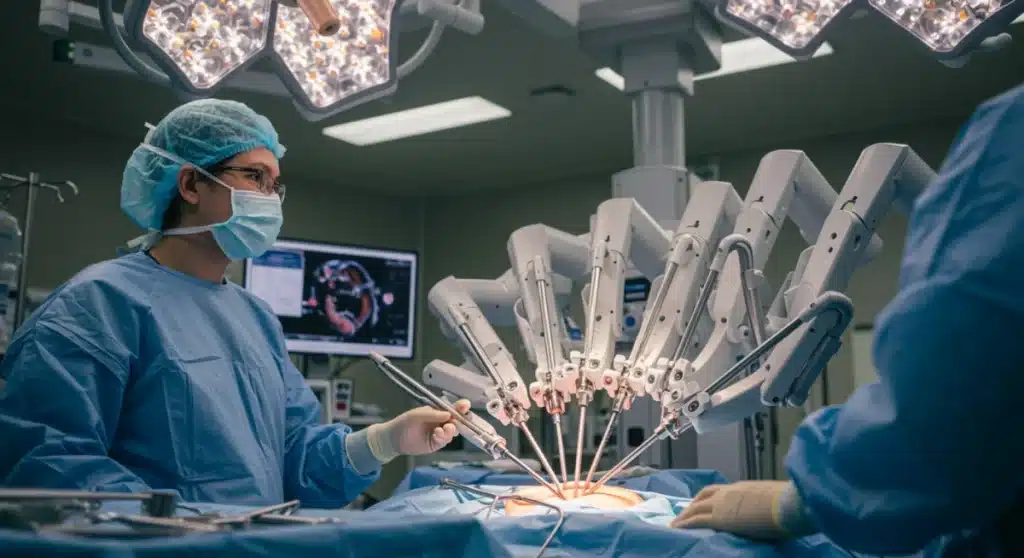
The landscape of modern medicine is undergoing a profound transformation, driven by an unyielding pursuit of precision, efficiency, and enhanced patient safety. At the forefront of this revolution lies the integration of advanced robotics in healthcare, particularly within the realm of surgery. The promise is not merely incremental improvement but a paradigm shift that could redefine surgical outcomes. Indeed, industry experts and technological forecasts suggest a staggering 20% reduction in surgical errors in U.S. hospitals by 2026, a testament to the burgeoning capabilities of next-gen robotic systems. This ambitious yet achievable goal underscores the critical role that Robotics Healthcare Surgical Errors mitigation will play in the coming years.
For decades, human hands, though highly skilled, have been the primary instruments in the operating room. However, the inherent limitations of human dexterity, endurance, and susceptibility to fatigue have always posed challenges, occasionally leading to complications. Robotic surgical systems offer a compelling solution, extending the surgeon’s capabilities beyond what is humanly possible. These sophisticated machines provide unparalleled precision, enhanced visualization, and superior control, factors that are directly correlated with a decrease in adverse events during surgical procedures.
The journey towards this 20% reduction is paved with innovation, rigorous testing, and widespread adoption. It involves not just the development of more advanced robots but also the comprehensive training of surgical teams, the refinement of surgical protocols, and a deeper understanding of human-robot interaction. This article will delve into the multifaceted aspects of this technological evolution, exploring the specific ways Robotics Healthcare Surgical Errors are being addressed, the benefits they bring, the challenges that need to be overcome, and the promising future they herald for patient care.
The Evolution of Robotic Surgery: From Da Vinci to Next-Gen Systems
The concept of using machines to assist in surgery is not entirely new. The ‘Arthrobot’ in 1983 marked an early foray, followed by the groundbreaking ‘PROBOT’ for prostate surgery in 1991. However, it was the introduction of the da Vinci Surgical System in 2000 that truly democratized robotic surgery, bringing it to the forefront of medical practice. The da Vinci system, with its magnified 3D vision and wristed instruments, allowed surgeons to perform complex minimally invasive procedures with greater precision and control than traditional laparoscopic techniques.
While the da Vinci system revolutionized surgical approaches, it also laid the groundwork for the next generation of robotic platforms. These newer systems are characterized by several key advancements. They often feature smaller, more flexible instruments, haptic feedback (allowing surgeons to ‘feel’ tissue resistance), and even autonomous or semi-autonomous functions for certain repetitive tasks. The push for next-gen Robotics Healthcare Surgical Errors reduction is driving innovation in areas such as:
- Artificial Intelligence (AI) and Machine Learning (ML): Integrating AI allows robots to learn from vast datasets of surgical procedures, identifying patterns and predicting potential complications. This can lead to real-time guidance for surgeons, flagging deviations from optimal pathways.
- Enhanced Visualization: Beyond 3D, new systems offer augmented reality (AR) and virtual reality (VR) overlays, projecting critical patient data, anatomical structures, and even pre-operative scans directly onto the surgical field. This ‘x-ray vision’ significantly reduces the chances of collateral damage.
- Miniaturization and Flexibility: Smaller, more articulate robots can access confined spaces within the body with less tissue disruption, leading to smaller incisions, reduced pain, and faster recovery times.
- Tele-surgery Capabilities: The ability to perform surgery remotely, connecting expert surgeons with patients in underserved areas, is becoming a reality, further democratizing access to high-quality care and potentially reducing errors due to lack of local expertise.
- Haptic Feedback Systems: Providing tactile feedback to the surgeon, mimicking the feel of tissue, helps prevent excessive force and improves the surgeon’s understanding of the surgical field, thereby reducing the risk of tissue damage.
These advancements are not just about making surgery easier; they are fundamentally about making it safer and more effective. By addressing the subtle nuances of human performance, next-gen robotic systems are directly targeting the root causes of surgical errors.
Understanding Surgical Errors and How Robotics Intervenes
Surgical errors, though rare, can have devastating consequences for patients. They encompass a wide range of incidents, from wrong-site surgery and retained surgical instruments to nerve damage and complications arising from imprecise movements. The causes are often multifactorial, including human fatigue, stress, lack of experience, poor communication, and inadequate visualization.
Robotics intervenes in several critical ways to mitigate these risks, directly impacting the reduction of Robotics Healthcare Surgical Errors:
- Precision and Stability: Robotic arms eliminate natural hand tremors and provide a steadier platform for instruments, allowing for movements with sub-millimeter accuracy. This is particularly crucial in delicate procedures involving nerves, blood vessels, or small organs.
- Enhanced Visualization: Robotic systems typically offer highly magnified, high-definition 3D views of the surgical field. This superior visualization allows surgeons to identify anatomical structures more clearly, differentiate between healthy and diseased tissue, and navigate complex regions with greater confidence.
- Improved Ergonomics: Surgeons operate from a console, often seated comfortably, reducing physical fatigue during long procedures. This improved ergonomic setup can help maintain focus and reduce the likelihood of errors caused by exhaustion.
- Wider Range of Motion: Robotic instruments often have more degrees of freedom than the human wrist, allowing for intricate maneuvers in tight spaces that would be impossible with traditional laparoscopic tools. This expanded range of motion reduces the need for larger incisions and minimizes tissue manipulation.
- Standardization and Automation: For certain repetitive or highly standardized tasks, robotic systems can be programmed to perform them with consistent accuracy. While full autonomy in surgery is still a distant prospect, semi-autonomous functions can reduce variability and human error in specific steps.
- Data Collection and Analysis: Modern robotic systems collect vast amounts of data during each procedure. This data can be analyzed to identify best practices, pinpoint areas for improvement, and even provide personalized training feedback to surgeons, further contributing to the reduction of Robotics Healthcare Surgical Errors.
The Projected 20% Reduction: What Does It Mean?
The prediction of a 20% reduction in surgical errors in U.S. hospitals by 2026 is a significant milestone. To put this into perspective, even a small percentage reduction in surgical errors can translate into thousands of lives saved, millions of dollars in healthcare costs averted, and countless instances of improved patient outcomes and quality of life. This projection is not just a hopeful estimate; it is based on several converging factors:
- Increasing Adoption: The number of hospitals adopting robotic surgical systems is steadily growing. As more surgeons become trained and comfortable with the technology, its benefits will spread across a wider patient population.
- Technological Maturation: As discussed, the technology itself is becoming more sophisticated, addressing previous limitations and introducing new capabilities that directly target error reduction.
- Improved Training and Education: Comprehensive training programs for surgeons and surgical teams are evolving, ensuring that operators are proficient in using these advanced systems effectively and safely.
- Integration with AI and Data Analytics: The ability to leverage AI for predictive analytics, real-time guidance, and post-operative analysis will significantly enhance decision-making and performance in the operating room.
- Economic Incentives: The long-term cost savings associated with reduced complications, shorter hospital stays, and lower readmission rates provide a strong economic incentive for hospitals to invest in robotic technology and improve patient safety, thereby focusing on Robotics Healthcare Surgical Errors prevention.
This 20% reduction represents a tangible improvement in patient safety, moving closer to the ideal of zero preventable harm in healthcare. It signifies a future where surgical interventions are not only effective but also remarkably safe, thanks to the symbiotic relationship between human expertise and robotic precision.
Benefits Beyond Error Reduction: A Holistic Impact
While the reduction of Robotics Healthcare Surgical Errors is a primary driver, the benefits of robotic surgery extend far beyond this crucial aspect. The holistic impact on patients, surgeons, and the healthcare system as a whole is transformative:
- For Patients:
- Minimally Invasive Procedures: Leads to smaller incisions, less pain, reduced blood loss, and lower risk of infection.
- Faster Recovery Times: Patients often experience quicker healing and can return to their daily activities sooner.
- Shorter Hospital Stays: Reduced complications and faster recovery translate to less time spent in the hospital.
- Improved Cosmetic Outcomes: Smaller incisions result in less noticeable scarring.
- Better Clinical Outcomes: In many cases, robotic surgery leads to superior functional outcomes, especially in complex procedures.
- For Surgeons:
- Enhanced Precision and Control: As mentioned, robots provide unparalleled dexterity and stable instrument control.
- Superior Visualization: High-definition 3D vision with magnification offers a clear and detailed view of the surgical field.
- Improved Ergonomics: Reduces physical strain and fatigue, allowing surgeons to perform longer and more complex procedures with sustained focus.
- Access to Difficult-to-Reach Areas: Robotic instruments can articulate in ways human hands cannot, enabling access to challenging anatomical locations.
- Training and Learning Opportunities: Robotic systems often include simulation features for training new surgeons and practicing complex cases.
- For Hospitals and Healthcare Systems:
- Increased Efficiency: Streamlined procedures and faster patient turnover.
- Cost Savings: Reduced complications lead to lower re-admissions and overall treatment costs in the long run.
- Enhanced Reputation: Offering cutting-edge robotic surgery can attract more patients and top surgical talent.
- Data-Driven Improvement: The ability to collect and analyze surgical data helps in continuous quality improvement and research.
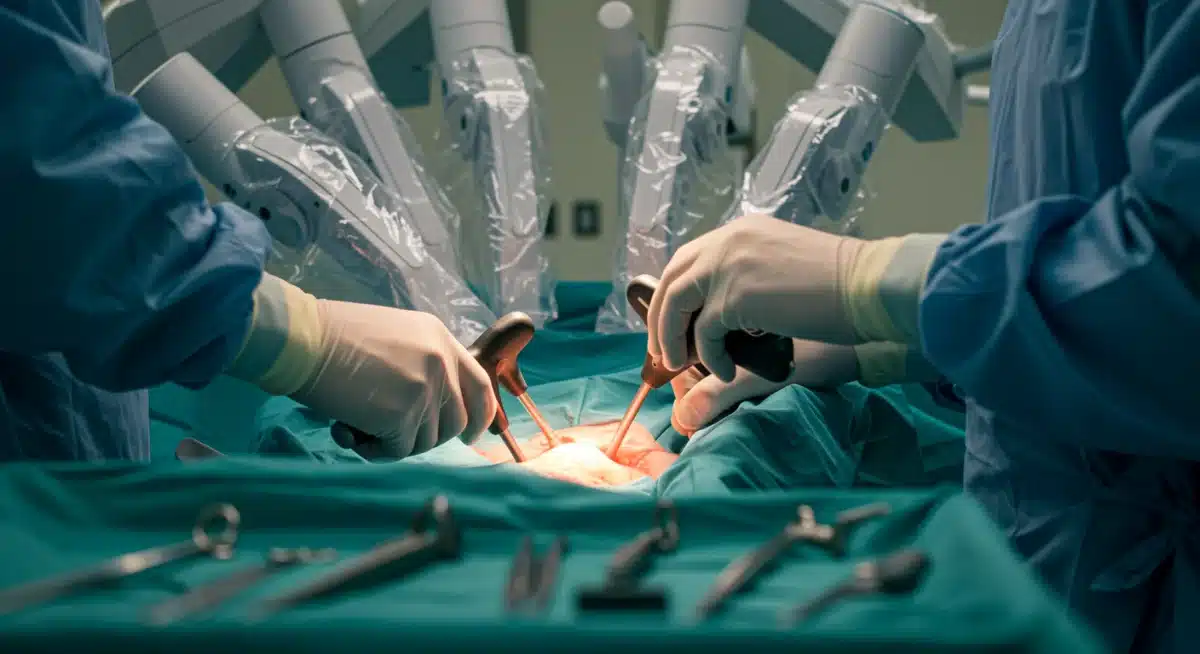
Challenges and Considerations for Widespread Adoption
Despite the undeniable advantages and the promising future of Robotics Healthcare Surgical Errors reduction, several challenges must be addressed for widespread and equitable adoption:
- High Initial Cost: Robotic surgical systems represent a significant capital investment for hospitals, which can be a barrier for smaller or less affluent institutions. The cost of instruments and maintenance also adds to the operational expenses.
- Training and Credentialing: While training is improving, ensuring that all surgeons are adequately trained and credentialed to use these complex systems requires substantial resources and standardized protocols.
- Learning Curve: There is a learning curve associated with mastering robotic surgery, and initial procedures may take longer. Adequate mentorship and practice are crucial.
- Ethical and Legal Implications: As robots become more autonomous, questions arise regarding liability in the event of an error. Defining the roles and responsibilities of human surgeons and robotic systems is an ongoing discussion.
- Data Security and Privacy: The collection of vast amounts of surgical data necessitates robust cybersecurity measures to protect patient information.
- Accessibility and Equity: Ensuring that the benefits of robotic surgery are accessible to all patients, regardless of their socioeconomic status or geographic location, is a critical challenge. The ‘digital divide’ in healthcare could be exacerbated if not proactively addressed.
- Integration with Existing Infrastructure: Seamless integration of robotic systems with hospital IT infrastructure, electronic health records, and other medical devices is essential for optimal performance and data flow.
- Over-reliance and Deskilling: There’s a concern that an over-reliance on robotics could lead to a decline in traditional surgical skills. A balanced approach, emphasizing the robot as a tool rather than a replacement for human expertise, is vital.
Addressing these challenges requires a collaborative effort from technology developers, healthcare providers, policymakers, and regulatory bodies. Investing in research, developing cost-effective solutions, and establishing clear guidelines will be crucial for realizing the full potential of robotics in healthcare.
The Future of Robotics in Healthcare: Beyond the Operating Room
The trajectory of robotics in healthcare extends far beyond its current applications in surgery. The innovations aimed at reducing Robotics Healthcare Surgical Errors are just the beginning. The future promises even more profound integrations:
- Diagnostic Robotics: Robots equipped with advanced sensors and AI could assist in more accurate and earlier disease diagnosis, performing tasks like biopsies or endoscopies with greater precision.
- Rehabilitation Robotics: Exoskeletons and robotic assistance devices are already helping patients with mobility impairments regain function and improve their quality of life. This field is expected to expand significantly.
- Assisted Living and Elder Care Robotics: Robots could assist the elderly with daily tasks, provide companionship, monitor health, and alert caregivers in emergencies, allowing them to maintain independence longer.
- Drug Discovery and Pharmacy Automation: Robots are already used in laboratories for high-throughput screening in drug discovery and for automating pharmacy tasks, reducing human error in medication dispensing.
- Micro- and Nanorobotics: The development of incredibly small robots capable of navigating the human body at a cellular level holds immense potential for targeted drug delivery, minimally invasive diagnostics, and even repairing damaged tissues from within.
- Personalized Medicine: Robotic systems, combined with AI, will play a crucial role in tailoring treatments to individual patient needs, analyzing vast genomic and proteomic data to recommend the most effective interventions.
- Robotic Nurses and Assistants: While not replacing human empathy, robots could take on repetitive, physically demanding, or hazardous tasks, freeing up human nurses and medical staff to focus on direct patient care and complex decision-making.
The pace of technological advancement suggests that many of these applications are not distant dreams but rather imminent realities. The ethical frameworks, regulatory guidelines, and societal acceptance will need to evolve in parallel to ensure these innovations are deployed responsibly and equitably.
Case Studies and Success Stories in Robotic Surgery
Numerous success stories already highlight the impact of Robotics Healthcare Surgical Errors mitigation. Hospitals worldwide have reported significant improvements in patient outcomes across various specialties:
- Prostatectomy: Robotic-assisted prostatectomy has become the gold standard for prostate cancer surgery, leading to better nerve-sparing outcomes and reduced rates of incontinence and impotence compared to open surgery.
- Gynecological Procedures: Hysterectomies and myomectomies performed robotically often result in less pain, smaller scars, and quicker recovery for patients.
- Cardiac Surgery: Minimally invasive robotic cardiac procedures, such as valve repair, reduce the need for large chest incisions, leading to faster recovery and fewer complications.
- Colorectal Surgery: Robotic platforms enable surgeons to navigate the confined spaces of the pelvis with greater ease, leading to improved outcomes for colorectal cancer resections.
- Head and Neck Surgery: Transoral Robotic Surgery (TORS) allows for the removal of certain head and neck tumors through the mouth, avoiding external incisions and greatly reducing morbidity.
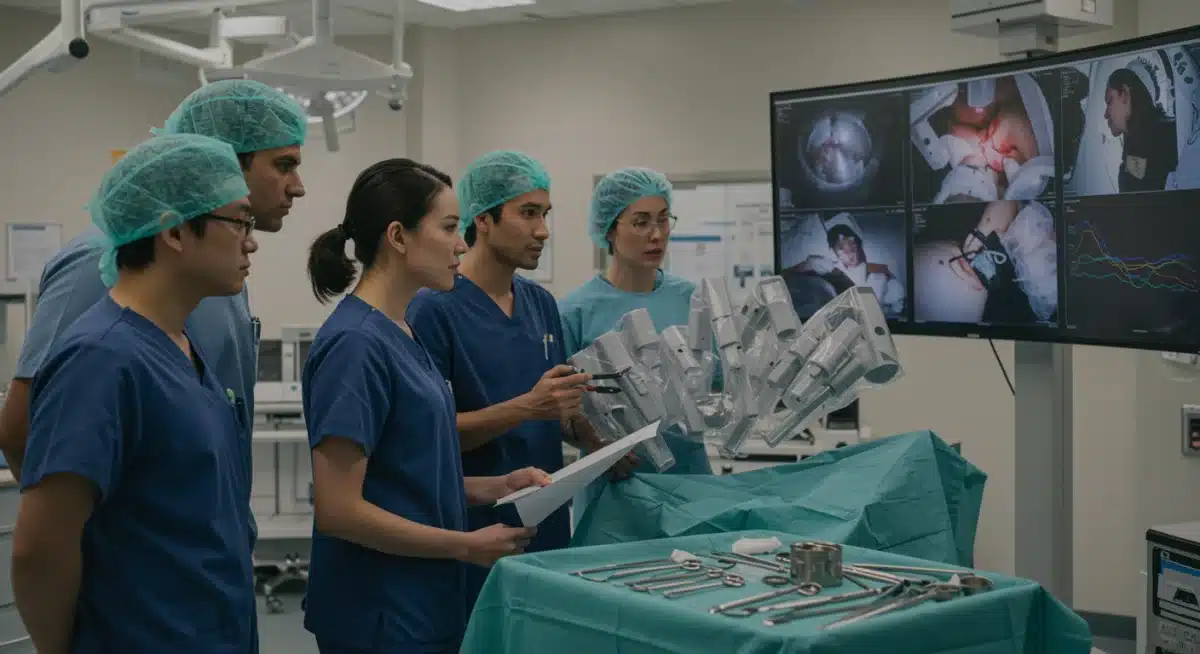
Preparing for the Future: Recommendations for Healthcare Providers
To fully capitalize on the projected 20% reduction in Robotics Healthcare Surgical Errors and embrace the broader benefits of robotic technology, healthcare providers should consider the following recommendations:
- Strategic Investment: Develop a clear strategy for investing in robotic systems, considering long-term benefits, return on investment, and patient population needs.
- Comprehensive Training Programs: Establish robust training and credentialing programs for surgeons, nurses, and support staff to ensure proficiency and safety.
- Interdisciplinary Collaboration: Foster collaboration between surgical teams, biomedical engineers, IT professionals, and data scientists to optimize the use and integration of robotic systems.
- Outcome Tracking and Data Analysis: Implement systems for meticulous tracking of surgical outcomes, complications, and efficiency metrics to continuously evaluate and improve robotic surgery programs.
- Patient Education: Educate patients about the benefits and risks of robotic surgery, helping them make informed decisions about their treatment options.
- Research and Development: Support ongoing research into new robotic applications, AI integration, and improvements in surgical techniques.
- Ethical Frameworks: Proactively engage in discussions and develop internal guidelines regarding the ethical and legal implications of increasing robotic autonomy.
- Focus on Human-Robot Teaming: Emphasize the concept of human-robot collaboration, where the robot augments human skill rather than replaces it, maintaining the surgeon’s ultimate responsibility.
By proactively addressing these areas, U.S. hospitals can not only achieve the ambitious goal of a 20% reduction in surgical errors but also position themselves at the forefront of medical innovation, delivering safer, more efficient, and more effective care to patients.
Conclusion
The promise of a 20% reduction in surgical errors in U.S. hospitals by 2026, driven by next-gen Robotics Healthcare Surgical Errors mitigation, is a testament to the transformative power of technology in medicine. From enhanced precision and visualization to improved ergonomics and AI-driven insights, robotic systems are fundamentally reshaping the operating room. While challenges such as cost, training, and ethical considerations remain, the trajectory of innovation is clear. The future of healthcare will be increasingly defined by the symbiotic relationship between human expertise and robotic capabilities, leading to a new era of unprecedented patient safety and clinical excellence. Embracing this future responsibly and strategically will be paramount for healthcare providers striving to deliver the best possible care.





